The purpose of this blog is to discuss cervical radiculopathy, which people sometimes refer to as a “pinched” nerve in the neck.
Do you have new, lingering, or recurring neck or thoracic symptoms that’s stopping you from doing the things you enjoy or keeping you from feeling like yourself? Check out our Neck & Thoracic Resilience Program!
Anatomy & Function
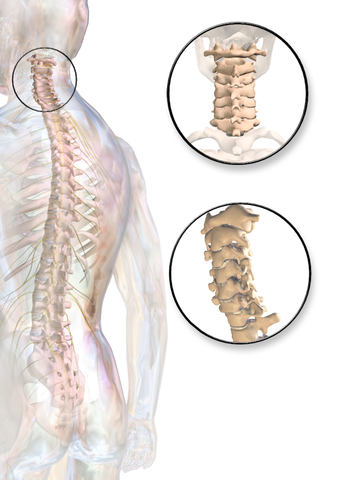
The cervical spine refers to the neck, which consists of seven vertebrae, or bones, with intervertebral discs spaced between them. Within this region of the spine is a portion of the spinal cord and its associated nerves that provide control and sensation to various structures, including your arms and hands.
The primary motions of the cervical spine are:
- Flexion – bringing your chin to your chest
- Extension – looking up toward the ceiling or sky
- Rotation – looking to the left and right
- Side Bend – bringing your left ear to your left shoulder and right ear to your right shoulder
- Protraction – imagining you’re trying to read small text on your phone
- Retraction – pulling your head back from something that smells awful

Cervical Radiculopathy
Cervical radiculopathy refers to neurological changes, such as numbness and weakness in the arms and hands, due to an issue originating in the neck – most commonly a herniated disc or degenerative changes that encroach on a nerve.
Typical signs and symptoms may include, but are not limited to:
- Numbness, burning, or tingling
- Muscle weakness
- Pain in the neck or arms (radicular pain)
- Loss of range of motion
Two important things to note:
1. These signs and symptoms occur along a continuum. For example, one person may present with no noticeable muscle weakness, while someone else may demonstrate significant atrophy of the affected muscles.

Goal of Rehab
Although symptoms associated with the neck or nerves are worrisome for a lot of people, there’s actually some really great news!
- Cervical radiculopathy has a favorable natural history, which means that it often gets better on its own, including changes in strength or sensation, regardless of the treatment implemented.
- “Abnormal” findings on imaging, such as disc herniations, bulges, stenosis, and various forms of degeneration, are quite common in people with no symptoms. Kuijper et al in 2011 also found that it’s possible, and quite common, to have compression of a nerve without having symptoms at that level. Imaging isn’t destiny.
Therefore, the purpose of rehab isn’t to change what your spine or structures look like on imaging. The goal is to improve your function and quality of life by improving your tolerance to various movements.
Understanding & Monitoring Symptoms
It’s important to monitor and understand fluctuations in symptoms during the management of cervical radiculopathy. For simplicity, I’ll compare it to an acute ankle sprain. Ask yourself 2 questions:
- Is my pain tolerable during exercise? If it’s helpful for you, you can rate your pain or discomfort on a scale from 0-10 and determine the highest acceptable number for you. You get to decide, but more isn’t always better. You’re not trying to “release” anything or find a quick fix. In the example of an ankle sprain, you want to get things moving in a comfortable manner while the body does what it’s supposed to do with regards to healing.
- Is my pain better, worse, or the same the day after exercise? If you notice a flare-up the following day, you might have done a little too much. In the example of an ankle sprain, maybe you have an increase in swelling or more difficulty with bearing weight. Not a big deal. That’s just information for you to use to modify what you’re doing, so you can find a more appropriate dosage of exercise.

Activity & Lifestyle Modifications
Specific exercises aren’t the only things to consider during the management of cervical radiculopathy. In fact, there’s no best exercise or intervention, but I’m trying to provide an approach that’s comprehensive. Here are 4 other things to assess:
- Sleep. How’s your sleep quality and quantity? A bad night of sleep can worsen your pain the next day.
- Stress. Do you notice any associations between stress or anxiety and your symptoms?
- Posture. There’s a common misconception that neck or nerve issues need to be fixed by always maintaining your shoulder blades down and back. However, constantly trying to put yourself in this position can actually exacerbate symptoms. There is no perfect posture, so explore what works well for you rather than trying to be rigid with your approach.
- Inactivity. How much of your day is spent sitting or looking at a screen? How does that influence your symptoms?
It would be unrealistic for me to ask you to make major changes in all of these categories. Instead, try to identify which of these might be contributing to your symptoms and reach for the lowest hanging fruit.
I haven’t been perfect, but here are 3 things that I’ve been trying to implement to improve my overall health:
- Consistent sleep schedule. I try to go to sleep at 10pm and wake up at 6am every single day.
- No phone use 2 hours upon waking and 2 hours before bed.
- Walking first thing in the morning and at least two 10 minute walks throughout the day.

Start with small wins and then add more over time if your chosen lifestyle changes are realistic and manageable.
Okay, time to discuss exercises. I’ve picked a few options that will help restore range of motion or strength lost due to disuse or deconditioning.
Isolated Neck Strength (Choose 1 Option)
Isometrics, in which little to no movement of the neck occurs, can be a useful starting point for isolated strengthening. Here are 3 options for flexion and extension:
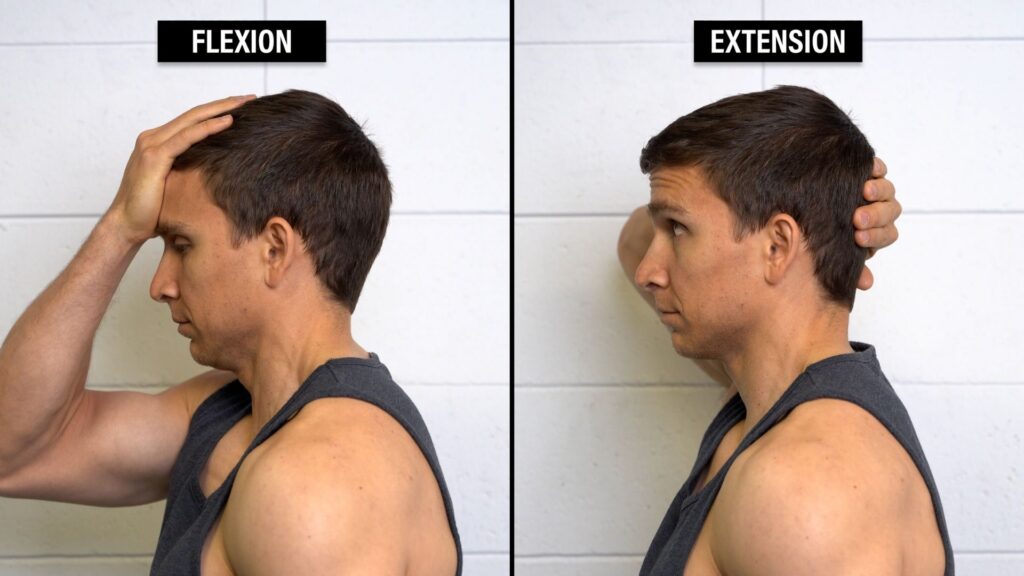
Option 1: Manual resistance. You can use your hands to resist flexion or extension of your neck. If you put your hand on your forehead and stop yourself from looking down, you are resisting neck flexion. If you put your hand on the back of your head and stop yourself from looking up, you are resisting neck extension. The goal is to find a tolerable starting point. If you resist as hard as you can, that’s 100%. Half of that is 50%. Half of that is 25%. You don’t need to go all out. Start with an estimated percentage that’s comfortable.
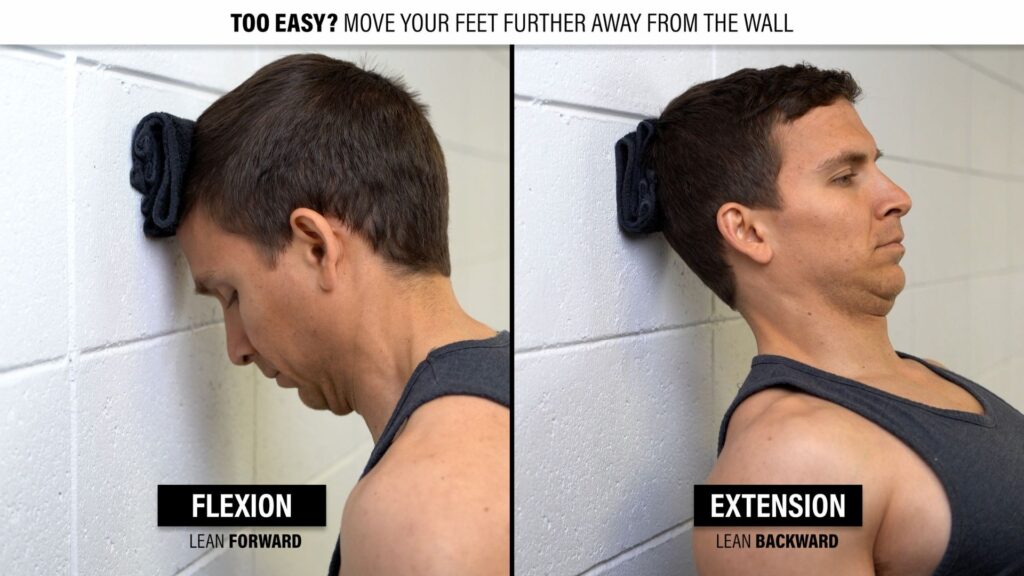
Option 2: Against a wall. You can use a towel, pillow, foam pad, exercise ball, etc. For flexion, you’ll lean forward against a wall with a slight chin tuck. For extension, you’ll lean backward against a wall with a slight chin tuck. The further you move away from the wall, the harder the exercise should be.
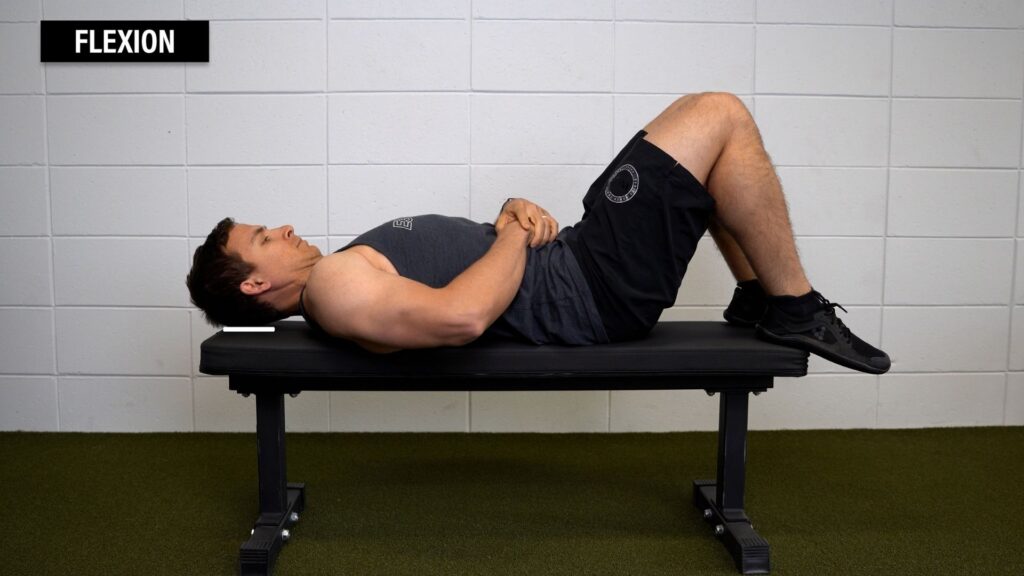
Option 3: On your back or all fours. For flexion, you can lie on your back, tuck your chin, and lift your head high enough to slide a piece of paper underneath it.
For extension, you can set up on all fours, slightly push the ground away from you, and imagine pulling your head back from an awful smelling item as mentioned earlier.

For the isometric exercises, you can pick one of the three options and try to accumulate 60 seconds of work, 3 times per day. You can do 1 set for 60 seconds, 2 sets for 30 seconds each, 6 sets for 10 seconds, etc. These can be done daily or every other day.

Integrated Neck Strength
You can achieve similar benefits by performing a comprehensive resistance training routine. I’ll demonstrate two options:
Option 1: Inverted Row. You can use a barbell or a suspension trainer. The more vertical you are, the easier the exercise. The more horizontal you are, the harder the exercise. You can choose a tolerable starting point and then progress over time. In addition to strengthening the muscles on the front of the neck, this exercise will strengthen your biceps, shoulders, and back.

Option 2: Push Up. You can progress from a wall to an elevated surface like a bench, and then to flat ground. You can go one step further by doing a push up to a downward dog.

If push ups are too challenging or uncomfortable, you can do planks in the same positions and then progress to a dolphin pose. In addition to strengthening the muscles on the front of the neck, this exercise will strengthen your triceps, shoulders, chest, and abdominals.

You can aim to perform 2-4 sets of 10-15 repetitions for each exercise, 2-3 times per week.

Cervical & Thoracic Rotation Range of Motion (1 Option)
The next category of exercises addresses cervical and thoracic rotation range of motion.
Option 1: Side Lying Thoracic Rotation – Lie on your side with your hips and knees bent, and head supported. Rotate your top shoulder and arm toward the floor behind you, or as far as you can comfortably go.
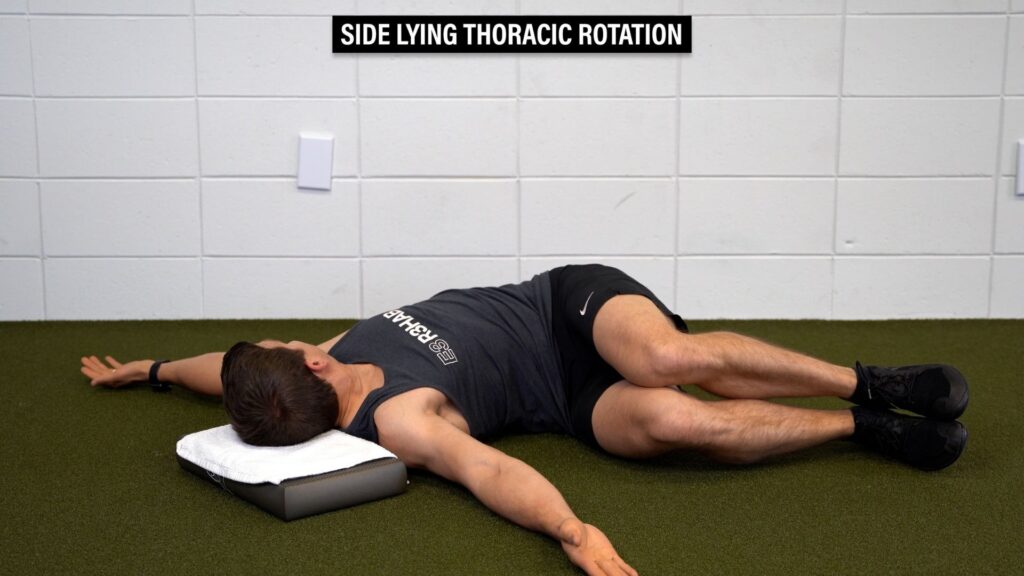
Option 2: Quadruped Thoracic Rotation – Sit back on your heels with your knees apart and hands out in front of you. Place one hand behind your head, rotate up toward the ceiling as far as you can comfortably go, and then rotate back the other direction.
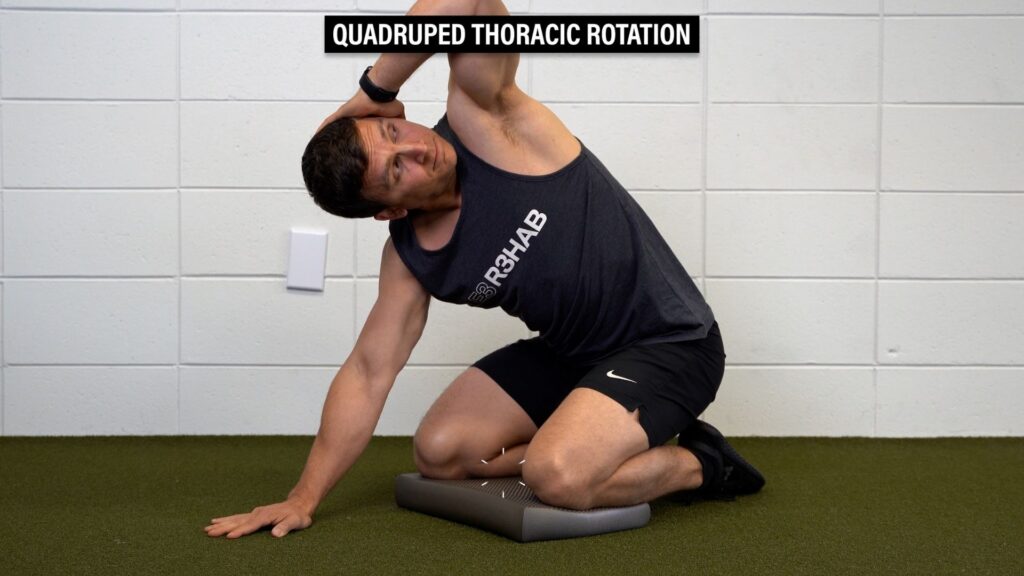
Option 3: Seated Thoracic Rotation – With your arms out in front of you, reach one hand toward the wall behind you, return to the starting position, and then repeat on the other side.
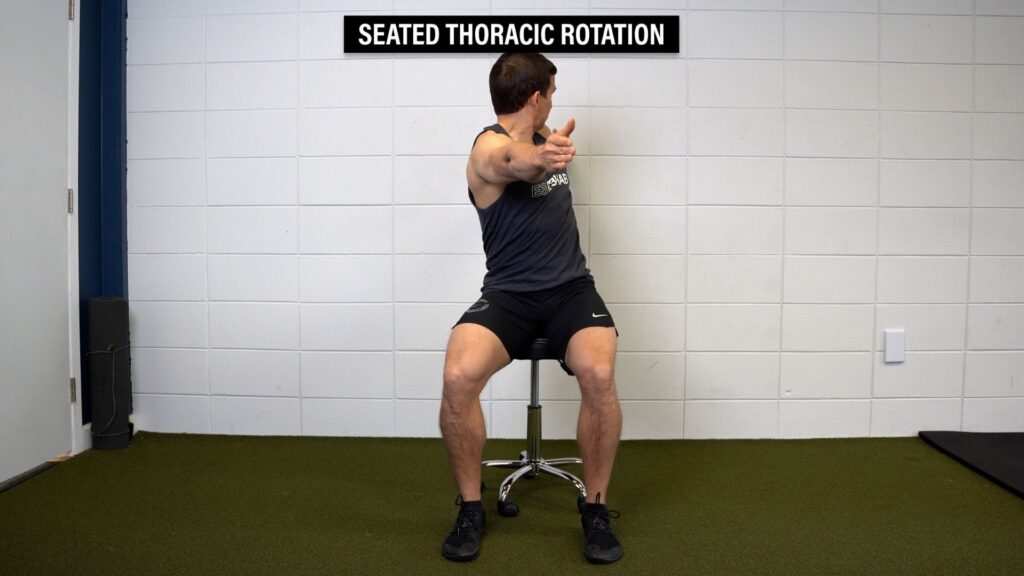
You can also lean forward, grab the opposite knee, and reach up toward the ceiling.
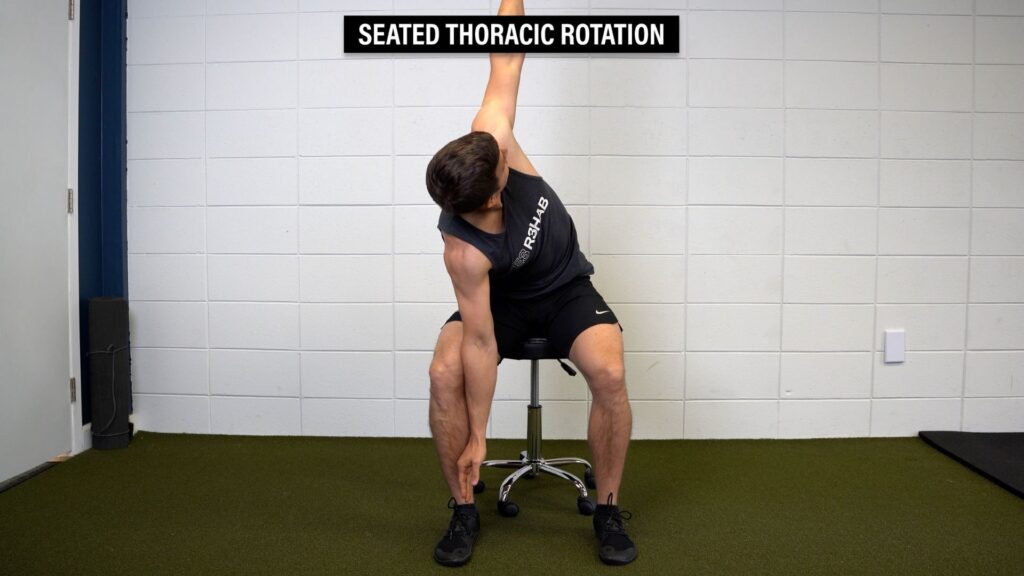
To make any of the movements easier or less intense, you can place your hand across your chest.
Determine which exercise feels best for you and perform it 2-3 times per day for 6-8 slow and controlled repetitions per side.

Cervical & Thoracic Flexion/Extension Range of Motion (1 Option)
The last category of exercises addresses cervical and thoracic flexion and extension range of motion.
Option 1: Quadruped Segmental Cat/Cow – Sit back on your heels with your knees apart and hands out in front of you. Tuck your chin, slowly bring it toward your chest, round your upper back, and work your way down as far as you can comfortably go. Then slowly reverse that motion. Option 2 is performing the same movement in sitting (seated cat/cow).
To make the movements easier or less intense, move slower and through a lesser range of motion.
Determine which exercise feels best for you and perform it 2-3 times per day for 3 to 5 slow and controlled repetitions.

Both categories of exercises are useful for introducing more movement into your daily routine if going for regular walks isn’t an option.

Guidelines, Not Rules
As always, this blog is providing guidelines, not hard and fast rules. The frequency, intensity, and volume of exercises need to be individualized based on your training history, symptoms, goals, etc. Some people may benefit from doing all the exercises while others do none of them, and instead focus on the activity and lifestyle modifications mentioned earlier.

When Should You Get Surgery?
I can’t give you a definitive answer, but I can provide you with information that you can take into consideration during that discussion with your medical doctor.
Persson et al in 1997 compared surgery, physical therapy, or a cervical collar for the treatment of cervical radiculopathy and concluded that “the 1-year outcome shows no significant differences between surgical and conservative therapy.”
Peolsson et al in 2013 and Engquist et al in 2013 compared surgery followed by physical therapy to physical therapy alone and found similar outcomes after 2 years. The authors concluded that “structured physiotherapy should be tried before surgery is chosen.”
Therefore, surgery may be indicated in some cases, such as when severe or progressive neurologic deficits are present, but non-operative management is usually the first recommendation.
To date, no randomized, placebo-controlled trials that compare real surgery to fake surgery have been conducted.
Summary
In summary, cervical radiculopathy refers to neurological changes, such as numbness and weakness in the arms and hands, due to an issue originating in the neck – most commonly a herniated disc or degenerative changes that encroach on a nerve. Other characteristics include pain, reduced range of motion, and symptoms in the scapular region. Since it has a favorable natural history and outcomes between surgical and nonsurgical treatment are similar, nonoperative management is usually the first recommendation.
Exercises should focus on improving function, such as strength and range of motion of the neck, upper back, and shoulders, rather than trying to change the structure of your spine. Additionally, it is important to consider how other lifestyle factors may contribute to your symptoms, such as diminished sleep quality or quantity, heightened stress, general physical inactivity, and sustained aggravating postures or positions.
Don’t forget to check out our Neck & Thoracic Resilience Program!
Want to learn more? Check out some of our other similar blogs:
Rhomboid Pain Exercises, Rhomboid Pain, Disc Herniations
Thanks for reading. Check out the video and please leave any questions or comments below.