The purpose of this blog is to discuss quadriceps strains, including the anatomy and function of the quads, how these injuries occur, and outline a rehab plan with exercises and criteria for returning to sport.
Looking to improve your strength, range of motion, and power to enhance your function and performance? Check out our Knee Resilience program!
Quadriceps Anatomy & Function
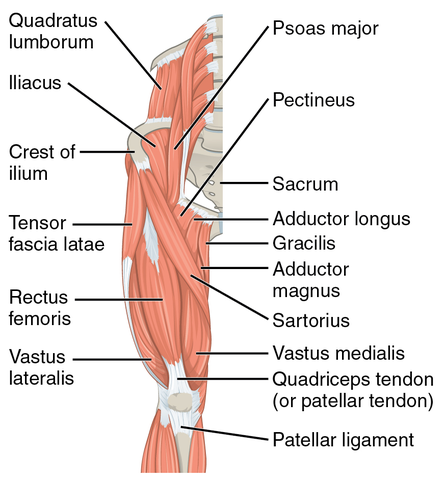
The quadriceps, as the name implies, consists of 4 different muscles – the vastus medialis on the inside of the thigh, the vastus lateralis on the outside of the thigh, the vastus intermedius deeper in the middle of the thigh (not shown), and the rectus femoris that sits right over the top. All four muscles insert on the tibial tuberosity via the patellar tendon and act to extend, or straighten, the knee. In fact, they are the only muscles that have this action. The rectus femoris also flexes the hip because its proximal attachment crosses this joint.
Rectus Femoris Muscle Injury
Due to its anatomy and function, the rectus femoris is the most commonly injured of the quadriceps muscle group. The injury occurs during sprinting or kicking, which is why soccer players are most affected – women more so than men.
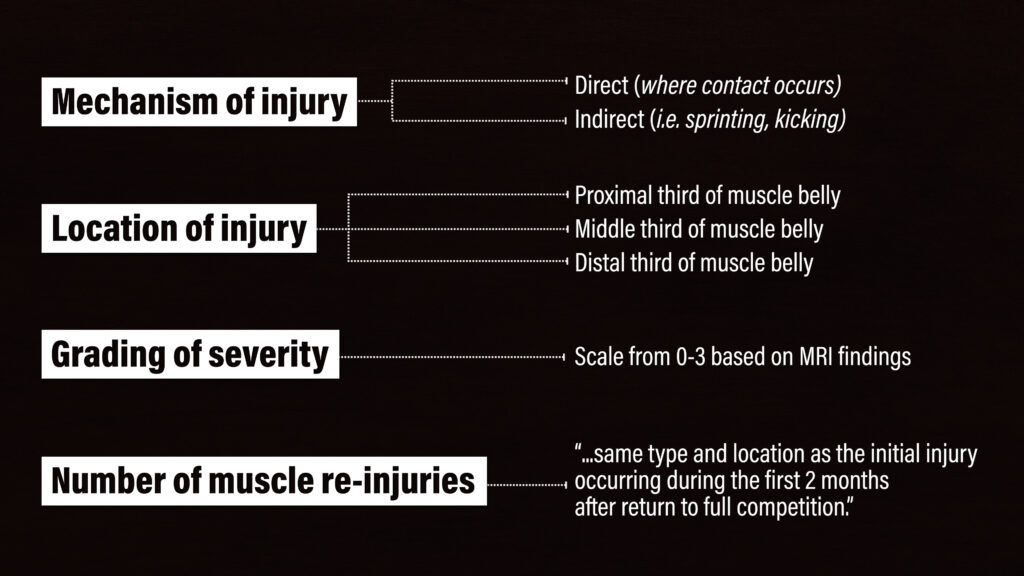
While muscle injuries may seem rather straightforward, there’s actually conflicting opinions on how they should be classified. The classification system by Valle et al in 2017 incorporates 4 categories: the mechanism of injury (M), location of injury (L), grading of severity (G), and number of muscle re-injuries (R).
The mechanism of injury is either direct (contact involved) or indirect. In this case, I’m discussing an indirect injury.
The location of injury is “subdivided into injuries located at the proximal, middle, or distal third of the muscle belly, with injuries further subclassified according to the relationship with the musculotendinous junction.”
Grading the severity of the injury is based on MRI findings on a scale from 0-3.
And “a recurrence is defined as an injury of the same type and location as the initial injury occurring during the first 2 months after return to full competition.”
This information is important because papers by Cross et al in 2004, Balius et al in 2009, and Brukner et al in 2016 have reported that prognosis is impacted by the location and extent of the initial injury. Additionally, Ekstrand et al in 2020 found that return to play timelines are longer after a re-injury.
However, my intention with presenting this information is NOT to encourage everyone to go out and get an MRI. Research by Wangensteen et al in 2015 and Jacobsen et al in 2016 recommend against routine MRI because it doesn’t necessarily provide additional value compared to a thorough clinical evaluation. Instead, I just think it’s important to understand that you shouldn’t compare your recovery timeline to a friend, family member, or professional athlete because circumstances vary considerably between individuals.
Quadriceps Strain Exercise Rationale
The common wisdom is that you need to rest and ice for at least a week after an injury, and that all exercise should be pain-free. However, research has begun to suggest otherwise.
Bayer et al in 2017 reported that “starting rehabilitation 2 days after injury rather than waiting for 9 days shortened the interval from injury to pain-free recovery and return to sports by 3 weeks without any significant increase in the risk of reinjury” in athletes with severe muscle injuries. Therefore, exercise can usually be implemented fairly quickly.
Exercise also doesn’t necessarily need to be pain-free for a successful outcome to occur. Hickey et al in 2020 concluded that “the conventional clinical practice of pain avoidance during acute hamstring strain injury rehabilitation may not be necessary” because results were similar between a group that underwent pain-free exercise compared to a group that was allowed to exercise up to a threshold of 4/10 pain.
Based on the anatomy and function of the rectus femoris, and the mechanism of injury during sprinting or kicking, rehab should emphasize exercises that target hip flexion and knee extension at moderate to long muscle lengths.
Research by Ema et al in 2016, Vigotsky and Bryanton in 2016, and Kubo et al in 2019 highlight the need to incorporate isolation exercises, as compound exercises that involve simultaneous hip and knee extension (squats, leg press, etc.) are insufficient for training the rectus femoris. Maeo et al in 2018 and Alonso-Fernandez et al in 2019 also demonstrate the benefit of eccentric muscle contractions.
Quadriceps Exercise Progression #1: Split Squat
The first exercise is a split squat progression which can improve knee flexion, hip flexion, and hip extension range of motion, as well as hip and knee extension strength.

Level 1 – Split Squat Isometric. Start in a stride stance and lower yourself straight down so that your back knee is hovering over an egg that you don’t want to crack. Focus on keeping your trunk upright and the distribution of weight relatively even between legs. Shorten the range of motion or use your hands if it’s too difficult. Aim for 3 sets of 60 seconds.

Level 2 – Rear Foot Elevated Split Squat Isometric. The overall technique of the movement and position of your torso should be similar, so use an object to elevate your back foot that isn’t too high. Keep an even distribution of weight between legs. Aim for 3 sets of 60 seconds.

Level 3 – Rear Foot Elevated Split Squat. You can actually alternate how you perform this exercise, especially if you’re struggling with the Reverse Nordic that I’m going to demonstrate next.

The first option is to place 70-80% of your weight through your lead leg and drive your knee as far forward over your toes as possible. Aim for 3-4 sets of 6-12 repetitions with a 3 second lowering phase and 2 second pause at the bottom of each repetition. Add weight as needed.

The second option is to gradually place the majority of your weight through your back leg as you keep your trunk straight and bring your butt to your heel, or as far as you can comfortably go. Aim for 3-4 sets of 6-12 repetitions with the same slow and controlled tempo.

Quadriceps Exercise Progression #2: Reverse Nordic
The second exercise is the Reverse Nordic, which requires full knee flexion range of motion and the ability to kneel without pain. If you don’t meet those minimum requirements, start there.

For the set up, kneel on a pad, pillow, or towel with your feet flat on the ground.
To perform the exercise, maintain a straight line between your knees, hips, and shoulders as you slowly lean back before returning to the starting position.
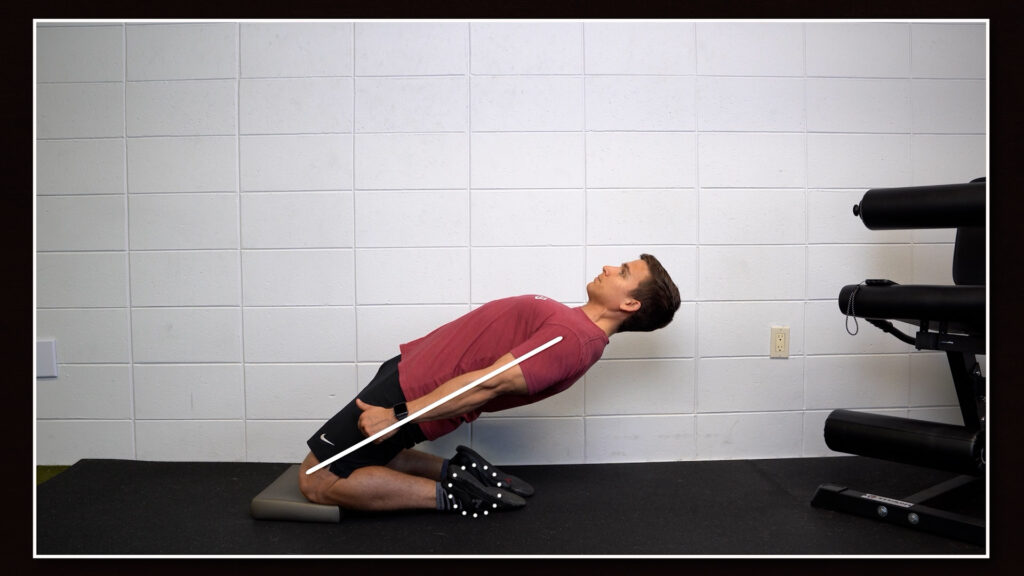
The easiest way to progress the exercise is to gradually increase the range of motion over time, and the easiest way to regress the exercise is to reduce the range of motion as needed.
You can either stack objects under your feet or set a target to tap as you slowly work your way to the ground.
Aim for 3-4 sets of 4-8 repetitions.

Quadriceps Exercise Progression #3: Hip Flexion
The last exercise progression is focusing on hip flexion.
Level 1 – Straight Leg Raise. Lie on your back with your hip and knee bent. With the opposite knee straight, squeeze your quads, and lift your leg until it’s approximately parallel with the other thigh before lowering back down. Aim for 3 sets of 20 repetitions. Repeat on both sides.

Level 2 – Straight Leg Raise with Knee to Chest. The overall movement is the same except you’re going to hug your opposite knee to your chest. Aim for 3 sets of 20 repetitions.

Level 3 – Straight Leg Raise with Knee to Chest on Elevated Surface. You’re now going to execute the exercise off the edge of a bed or table to increase the hip extension range of motion. Aim for 3-4 sets of 10-15 repetitions with at least a 3 second lowering phase. Add resistance over time as needed.

Returning to Sport After a Quadriceps Strain
Although the exercises will aid in your recovery, it’s essential that you also include and gradually progress the volume, frequency, and intensity of sport-specific movements, such as running, kicking, and jumping, to match the eventual demands of your sport. Additionally, setting objective goals for range of motion, strength, and functional tasks can help ensure that you return to sport safely while reducing your risk of re-injury. Here’s six criteria that you can take into consideration and work toward:
- No pain during the Ely Test, with knee flexion range of motion comparable to the uninjured leg

- No pain during the Thomas Test, with hip extension range of motion comparable to the uninjured leg

- No pain during a seated leg extension, with a 10 rep maximum equal to the uninjured leg
- No pain during resisted hip flexion, with a 10 rep maximum equal to the uninjured leg
- No pain or apprehension during sprinting at 100% effort
- No pain or apprehension during kicking at 100% effort

Guidelines, Not Rules
As always, the recommended exercises and progression criteria are based on guidelines, not hard and fast rules. Quadriceps exercises should be performed 2-3 times per week within a tolerable range of symptoms, but the process needs to be individualized based on your training history, goals, etc. Find a healthcare provider who can work with you during this process.

Myositis Ossificans
The last thing I want to mention is that if you have a palpable lump in the middle of your thigh, it’s not a trigger point that requires massage or foam rolling. A benign bone or bone-like tissue formation, known as myositis ossificans, can grow within skeletal muscle after an injury. Symptoms related to it normally resolve with conservative management, so it’s not usually a cause for concern. If you notice a bump or lump in your thigh, just bring it to the awareness of your physical therapist or medical doctor.
Don’t forget to check out our Knee Resilience Program!
Hamstring Strain Injury, Adductor Strain, Reverse Nordics
Thanks for reading. Check out the video and please leave any questions or comments below.